How Hantavirus Exposure Actually Happens

In the United States, hantavirus can only be transmitted from rodents to humans. There have been no confirmed cases of the Andes strain in the U.S., the one strain where human-to-human transmission is possible. But this rare disease risk is about more than just rodents. Americans have been exposed to hantavirus without ever seeing a mouse.
Exposure to hantavirus can happen through pathways that people often don’t think about. Hantavirus was the disease that killed Betsy Arakawa, the wife of actor Gene Hackman, in Santa Fe in early 2025. This disease killed three Mammoth Lakes residents in that same season. Hantavirus also closed and demolished 91 cabins at Yosemite in 2012 after ten visitors were infected, three of whom died. All three instances were the same illness, and most people wouldn’t have recognized the moments of exposure if they had been there to see them.
The disease also has a habit of finding healthy, active people doing routine things, and that is exactly what first caught researchers’ attention. This rare illness is better understood now, and the patterns behind exposure are recognizable. What is needed is for those patterns to be more widely known.
What Hantavirus Is & How It Spreads
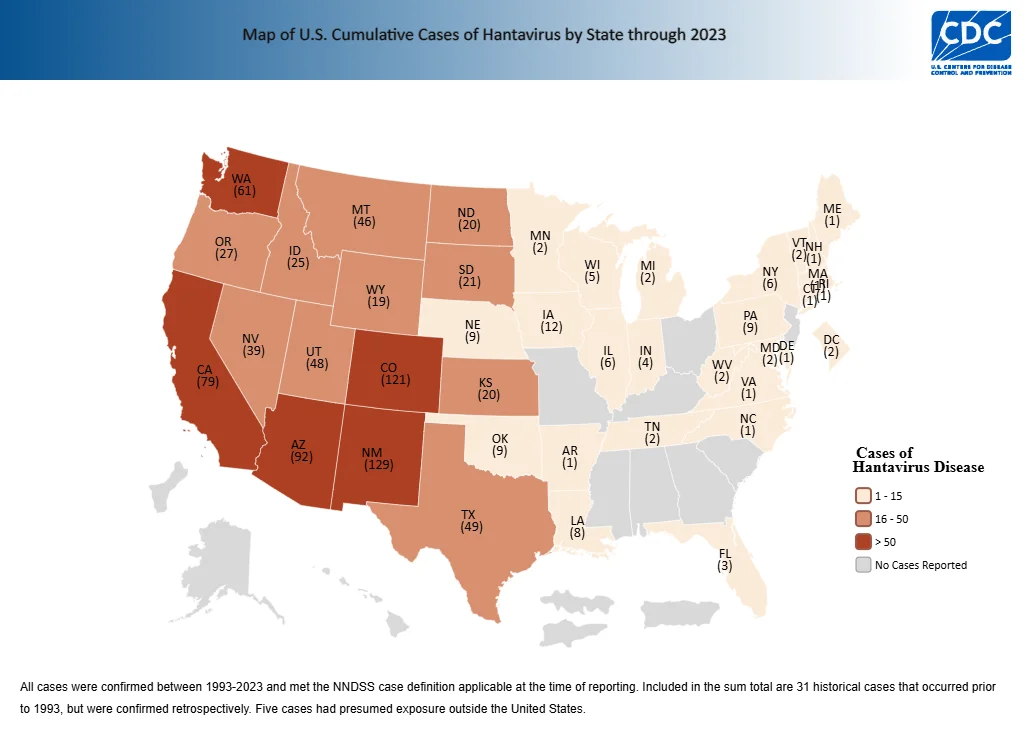
Hantavirus is a family of viruses that can be carried by certain types of rodents, which include the rice rat, white-footed mouse, cotton rat, and most notably, the deer mouse. In the U.S., the deer mouse is the primary carrier, and the strain that it carries is the Sin Nombre virus (SNV). The disease it causes here is hantavirus pulmonary syndrome (HPS). The CDC has tracked 890 confirmed hantavirus cases in the U.S. between 1993 and 2023, the overwhelming majority of them west of the Mississippi. The most reported cases are in the Four Corners region, especially Colorado, Arizona, and New Mexico, while California and Washington also have had a high number of confirmed cases.
There are multiple pathways to infection.
The most common pathway that accounts for most U.S. cases is inhalation of aerosolized particles from rodent urine, droppings, or saliva. This virus can also be contracted by touching contaminated surfaces and then one’s face, which can happen even while cleaning those surfaces, especially if one isn’t wearing gloves. You can also ingest this virus if you eat food that has been contaminated by rodent urine, droppings, or saliva. Finally, while rare, it is possible to contract a confirmed case of hantavirus by being bitten or scratched by an infected rodent.
A person can thus be exposed with or without seeing a rodent, or in some cases, without even being aware that they’ve deposited excrement or saliva in the area. A rodent’s infected saliva, urine, and droppings can be infectious for days. Moving stored items, stepping into a musty garage, or entering a cabin that’s been closed for the season can all be opportunities for unwitting exposure.
Common disturbances that aerosolize the virus include:
- Sweeping
- Vacuuming
- Shaking out blankets, tarps, sleeping bags
- Moving stored boxes
- Opening drawers, toolboxes, or storage bins that haven’t been touched in months
- Sorting through old gear
This is why the CDC explicitly warns against sweeping and vacuuming areas with potential or confirmed rodent activity. Both methods do exactly what the virus needs to infect someone: they put dried particles into the air at breathing height.
The locations linked to U.S. hantavirus cases form a recognizable list. Garages, sheds, and outbuildings are risk areas, as are cabins, hunting camps, and vacation properties. Storage units, basements, attics, crawl spaces, and walls have all been documented. Vehicles parked outdoors for extended periods carry their own risk, particularly in rural settings. Workplaces also matter, and not just the obvious ones, such as agriculture, ranching, construction, forestry, and parks outdoors. These risks can also be present in indoor environments like hotels, building maintenance operations, and resort and recreation businesses.
The Unclear Symptoms
Early symptoms of hantavirus are easy to confuse with influenza, COVID-19, or a stomach virus, as they start out as a fever, fatigue, severe muscle aches, and/or nausea, vomiting or diarrhea.
Hantavirus Symptoms and Treatment
No symptoms appear during this window.
Fever, fatigue, severe muscle aches, and often nausea, vomiting, or diarrhea.
Lungs fill with fluid. Breathing becomes labored. Patients can decline within hours.
No drug targets hantavirus directly. No approved vaccine exists in the U.S. for the strains that cause HPS in the Americas.
Hospitalization and oxygen support. ECMO at specialized facilities in severe cases.
Hantavirus pulmonary syndrome is fatal in about a third of cases. Survival depends largely on early supportive care.
If you develop flu-like symptoms after possible exposure to rodents, droppings, or a long-closed space, mention the exposure when you seek medical care. Early recognition is one of the few factors that can meaningfully change outcomes.
With the incubation period for hantavirus pulmonary syndrome being 1 to 8 weeks after exposure, most people don’t connect their symptoms to a cleaning task or anything they did weeks ago. After four to ten days of flu-like illness setting in, the disease can progress sharply. The fatality rate is about 35%, per the CDC (note that this rate refers to U.S. strains).
There is no specific antiviral treatment, and there is no vaccine. Survival depends almost entirely on early supportive care, and in severe cases, extracorporeal membrane oxygenation. This ECMO is a type of life support that does the heart and lungs’ work for them.
The Unexpected Victims
The Four Corners outbreak of 1993 was the event that led to hantavirus pulmonary syndrome being identified as a distinct disease. It was first noticed because young, otherwise healthy people were dying suddenly of what looked like a simple flu. One of these early cases was a 19-year-old Native American man, a competitive marathon runner of local renown, who became severely short of breath while traveling through New Mexico and died shortly after, just days after his fiancée, also a runner, had suddenly died with similar symptoms.
The virus would eventually be identified among dozens of other patients that year, 13 of whom died. This outbreak would later be linked to the Sin Nombre Virus (SNV), transmitted by the deer mouse. Researchers found that the victims’ households had more rodents than control households, and that these victims were often cleaning their homes or gardening. The activities that put these often young victims at risk were normal, even responsible.
The 2025 Mammoth Lakes cluster fits the same shape. The third confirmed death was a young adult, just 26 years old by some reports. According to the Mono County Public Health department, none of the three victims appeared to have engaged in activities that are typically associated with hantavirus exposure. One victim was said to have vacuumed in an area where mouse droppings were found. Their exposure across the board traced to ordinary daily life, homes and workplaces in a town where deer mice are common. In fact, the Eastern Sierra region is known to have a sizable deer mice population, and Mono County has the most recorded hantavirus cases in California since 1993 (27 confirmed reports).
How These Hantavirus Risks Can Stay Hidden
About one in three confirmed U.S. hantavirus cases involved a person who never observed a mouse.
Rodent nests can stay hidden inside walls, insulation, attics, crawl spaces, vehicle air systems, and the gaps behind appliances. The droppings, urine, and nesting material can all remain out of sight. In low-light and low-ventilation conditions, such as a cabin that has been closed up for the season, a virus can remain for days after an infected rodent has passed through. Dry surfaces in such conditions can still hold a viable virus without anyone knowing about the potential for exposure.
That also means that dried particles on a shelf, in a drawer, or on top of stored items can be invisible until they are stirred up. Visibility is not a reliable indicator of safety.
The Risks Build Up Before You Walk In
Long before a person opens a closed-up garage or moves a storage container, the conditions that could make the space dangerous have already been shifting.
Rodent populations tend to be weather-driven. Wet winters and springs increase plant productivity, which expands food supply for deer mice (and other hantavirus-carrying mice), which drives population booms several months later.
How Risk Builds Before You Walk In
The 1993 Four Corners outbreak followed this pattern. After several years of drought, heavy snowmelt and spring rains in early 1993 produced an unusually strong food supply, and researchers later traced the outbreak to a roughly tenfold increase in local deer mouse populations from the previous year. The El Niño Southern Oscillation event of 1991-1992 is the climate driver most often cited. A second El Niño event in 1997-1998 produced a roughly fivefold increase in hantavirus cases in the same Four Corners states in the following year. The link between rainfall, rodent populations, and human cases is one of the most consistent patterns noted.
Mono County’s public health also flagged in 2025 that local deer mouse numbers appeared elevated, which is consistent with the unusual February timing of the cluster. Cases historically peak in late spring and summer, when people return to spaces that rodents have been using through the cold months.
Whatever the weather and mouse population numbers might be, by the time someone walks into a shed, a rental cabin, or even their own garage in spring, the hantavirus risk may have been building for months. These are areas that need to be approached with caution, and careful cleanup processes.
How to Clean Up Safely
The good news is that household bleach, detergent soap, and disinfectants can easily kill hantavirus. Even sunlight and fresh air can be enough to deactivate the virus. However, the manner in which you go about cleaning an area where rodents have been present is vital.
How to Safely Clean Up After Rodents
As for disinfecting vehicles, bedding, carpets, books, and various surfaces and items, the CDC offers more specifics on how to do so safely.
Heavy Infestations Are a Different Category
For piles of droppings, multiple nests, dead rodents, or any space that has been closed up with active infestation for an extended period, the CDC recommends professional remediation rather than do-it-yourself cleanup. The risk profile of those environments is meaningfully higher.
Prevention Can Close the Loop
To prevent future intrusions of rodents, it is recommended that you seal exterior gaps larger than a pencil’s width. Caulking and steel wool, metal, and concrete are good plugs and seals, something that mice can’t gnaw on. Don’t leave food in your car, and don’t leave dirty dishes unwashed overnight. Store food in rodent-proof containers. Use snap traps rather than glue traps or live traps, which can frighten rodents into urinating and increase contamination.
Awareness, Recognition & Preparedness Are Key
Hantavirus has been a deadly risk in the U.S. since at least 1959, but it was only identified as a distinct disease in 1993. We now know more about this rare virus, and the risk to the public at large is still very low. But with the mortality rate that hantavirus carries, the risks must be taken seriously.
Hantavirus cases have been confirmed in most states in the contiguous U.S., yet some regions clearly have a much more significant rodent population that carries the virus. These areas are west of the Mississippi, especially concentrated around the 4 Corners region and the Sierra Nevadas. Certain seasons and conditions carry a higher risk of such rodents being active and reaching humans. Cleaning out areas or performing maintenance on long-undisturbed spaces need to be carried out with care and precision. Property owners who rent out cabins or homes need to be aware of seasons of heightened risk and how to safely deal with any mouse infestations before visitors are unknowingly exposed. Employers must also be aware of such health risks their workers face, have a written safety plan, and follow that plan.
The risks of hantavirus exposure are not exotic, and they don’t typically come from out-of-the-ordinary trips or behavior. For those who find themselves in higher-risk areas, however, this awareness and knowledge can be enough to recognize the patterns rather than walk into them.
When hantavirus exposure happens in a workplace, vacation rental, or other space someone reasonably trusted to be safe, the questions that follow are often about what conditions were known and what should have been done before anyone walked in. Arnold & Itkin’s hantavirus attorneys represented an oilfield worker’s family after he died as a result of hantavirus exposure, securing a $209 million verdict on their behalf. The firm’s trial lawyers have recovered more than $25 billion in verdicts and settlements for clients across the country, with a long record of holding corporations accountable when preventable conditions cause serious harm. Arnold & Itkin is based in Houston and represents clients in Texas and nationwide.


